
Nurses' Health and Workplace Exposures to Hazardous Substances
Caring for patients during a typical workday, nurses handle dozens of chemicals, drugs, and other agents that are designed to prevent, diagnose, control, or cure diseases and other health conditions. These therapeutic agents can heal, but have side effects as well. For most patients, the benefits of tightly controlled doses usually outweigh the risks. But the same may not be true for nurses.
Nurses absorb a small fraction of the substances they use to care for patients, day after day. They incur risks from these exposures in the absence of benefits. But the magnitude of health problems nurses may face from their diverse, chronic, workplace exposures to hazardous cleaning, disinfecting, and sterilizing agents, radiation, mercury, potent medications, and other chemicals has never been studied.
A new online survey of workplace exposures and disease conditions among 1,500 nurses was conducted by the Environmental Working Group (EWG) and Health Care Without Harm (HCWH), in collaboration with the American Nurses Association and the Environmental Health Education Center of the University of Maryland's School of Nursing, and supported by numerous state and specialty nursing organizations. Nurses were asked to provide information about their health, the health of their children, and about their exposures to 11 different common health care hazards.
This comprehensive survey shows that participating nurses who were exposed frequently to sterilizing chemicals, housekeeping cleaners, residues from drug preparation, radiation, and other hazardous substances report increased rates of asthma, miscarriage, and certain cancers, as well as increases in cancers and birth defects, in particular musculoskeletal defects, in their children. There are workplace safety standards for only six of the hundreds of hazardous substances to which nurses are exposed on the job.
Survey findings: Nurses' children, cancer, and birth defects
The many substances that nurses inhale, ingest, and absorb during a typical workday include some that are known or suspected to harm the development of a child in utero. In this survey, nurses report health problems in their children that are associated with exposures to an array of hospital hazards:
- Analysis of survey data shows that nurses' reported exposures during pregnancy to hazardous drugs, housekeeping chemicals, anesthetic gases, and disinfecting and sterilizing agents are associated with increased incidence of birth defects among their children (Figure 1).
- Children born to nurses reporting high exposures to these chemicals (at least once a week for nine months) were up to two times more likely to be born with a congenital defect than children born to nurses with low or no exposures to these agents, and up to nine times more likely to suffer from musculoskeletal defects at birth. Of the hundreds of compounds in these exposure categories, for only one has the government set standards specifically to restrict nurses' exposures (the sterilizing agent ethylene oxide).
- Nurses reporting high exposures to radiation during pregnancy (at least once a week for nine months) disclosed a 36 percent higher cancer incidence among their children than nurses exposed less often or not at all. The government does restrict allowable radiation doses for pregnant nurses. However, monitoring is infrequent, equipment can be faulty, and only the state of California mandates that the lowest possible effective doses be used for patients' X-rays and CT scans.
- These findings are consistent with other studies showing that children face risks from their mother's exposures to hazardous substances. Although the doses that cause harm are often not well-defined, a child in utero faces higher risks than the mother from hazardous exposures. EPA studies show that children are far more sensitive to carcinogens than adults (EPA 2005), and biomonitoring research demonstrates that chemicals linked to cancer and birth defects cross the placenta as readily as alcohol or cigarette residues (EWG 2005).
Figure 1. Nurses in the category of high exposure to hazardous hospital chemicals during pregnancy report elevated rates of birth defects among their children.
Comparative rates of birth defects in nurses' children, scaled to reflect the number of birth defects expected in a population of 1,000 nurses based on the findings of this study. Increased incidence of birth defects in children of nurses with high exposure, relative to those with low exposure, is listed above the bars representing high exposure.
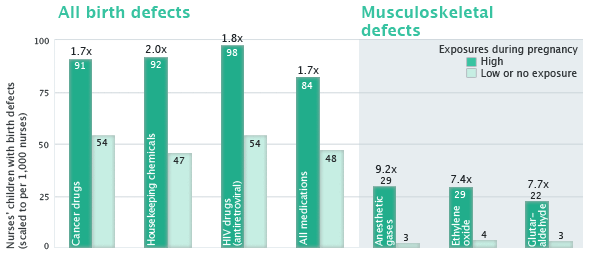
Notes: "High exposure" refers to reported exposure frequency of at least once weekly during pregnancy. "Low or no exposure" refers to all other, lower reported exposure frequencies. Birth defect rates reflect all congenital defects reported by surveyed nurses, with the exception of data shown for high level disinfecting and sterilizing agents (ethylene oxide and glutaraldehyde) and anesthetic gases, which apply to musculoskeletal defects only. See Table 1 for further details of survey findings, including sample sizes.
Survey findings — Do nurses' exposures affect their asthma, cancer, and miscarriage rates?
The 1,552 nurses who completed the survey reported a total of 730 different health conditions ranging from contact dermatitis to migraines, diabetes, and brain cancer. Analysis of the data revealed associations between a diverse range of reported exposures and health problems (Figure 2):
- Nurses reporting high exposures (at least once a week for at least 10 years) to medications of any type reported a 14 percent increase in cancer incidence relative to nurses with low or no exposure. For the nurses reporting high exposure to antineoplastic drugs, this jumped to an over 40 percent increase in cancer incidence relative to nurses with low or no exposure. In addition, nurses with high exposures to radiation disclosed a 20 percent higher incidence of breast cancer.
- Asthma rates increased by up to 50 percent for nurses reporting high exposures to disinfecting and sterilizing agents (glutaraldehyde and ethylene oxide), housekeeping chemicals, and latex, relative to nurses with lower exposures to these hazards.
- Nurses reporting high exposures to ethylene oxide and antineoplastic drugs also reported up to 20 percent higher incidence in miscarriage, on average, than nurses with lower or no exposure.
- Of the literally hundreds of compounds and agents in these exposure categories that are associated with health problems among nurses, for only six has the government set standards that could be used to limit nurses' exposures — radiation, mercury, isopropyl alcohol, the sterilizing agent ethylene oxide, and platinum- and arsenic-based drugs. For all remaining exposures, each health care facility decides what, if any, protective measures to require or recommend to control nurses' exposures to hazardous agents in the workplace.
Figure 2. Nurses report elevated rates of cancer, asthma, and miscarriage linked to their exposures to hazardous hospital chemicals and agents.
Comparative rates of cancer, asthma, and miscarriage in nurses, scaled to reflect the number of health conditions expected in a population of 1,000 nurses based on the findings of this study. Increased incidence of disease in nurses with high exposure, relative to those with low exposure, is listed above the bars representing high exposure.
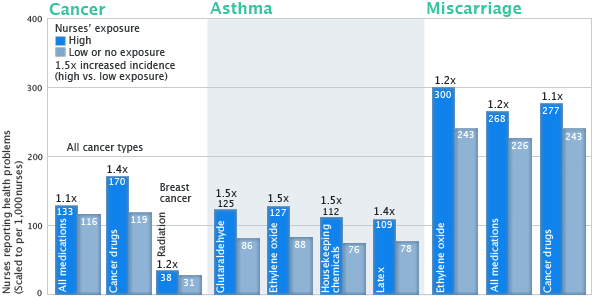
Notes: "High exposure" refers to reported exposure frequency of at least once a week for at least 10 years. "Low or no exposure" refers to all other, lower reported exposure frequencies. See Table 2 for further details of survey findings, including sample sizes.
Although these results are striking, this study has limitations. The group of participants that responded to the survey was not "controlled," or selected to meet any particular criteria — all nurses who learned of the survey through the publicity efforts of Health Care Without Harm, the American Nurses Association, the Environmental Health Education Center of the University of Maryland's School of Nursing, and other nursing organizations, were free to complete the online questionnaire. Though surveys are common means to collect information on health (e.g. Hemminki et al. 1982, Valanis et al. 1999, Mohan et al. 2003, Dimich-Ward et al. 2004, Yoshinaga et al. 2005, Delclos et al. 2006), research shows that self-selecting respondent pools would be expected to have higher than typical rates of health impacts, and to report higher exposures in cases where the respondent suspects an association with a health problem.
Another common issue when collecting health data via survey is the accuracy with which respondents report their medical conditions. Nurses are typically better educated about disease and health than the general population, and therefore may provide more accurate information via survey, but such "reporting bias" must be considered when reviewing this data. Analytical decisions regarding classification of the nurses into high and low exposure categories may also affect survey interpretation.
Survey analysis did not control for possible confounding factors like a nurses' exposure to multiple chemicals linked to common health effects, or for factors that often influence health, such as age, smoking and drinking habits, and day or night shift work. In particular, this study did not take into consideration the impact of mixed or combined chemical exposures, a serious issue because most nurses are exposed to multiple chemicals in the workplace at the same time. There is a critical need for research on the effects of multiple chemicals and hazardous agents interacting within the human body, similar to studies typically performed to investigate the potential impacts of combinations of medications on human health.
Yet despite these potential biases and limitations, these survey findings are remarkably consistent with laboratory and occupational studies of the hazardous agents investigated. While this survey does not provide definitive answers on health risks faced by nurses and their children, it does illustrate the critical need for standards that limit nurses' exposures to hazardous substances. It also demonstrates the necessity of a comprehensive, national study of nurses' health and exposures to chemicals and other hazardous materials.
Survey methodology
In collaboration with Health Care Without Harm, the American Nurses Association, and the Environmental Health Education Center of the University of Maryland's School of Nursing, Environmental Working Group scientists designed an online survey to assess the relationships between nurses' health and their exposures to 11 different common health care hazards. Health Care Without Harm, the American Nurses Association, and other collaborating nursing organizations publicized the survey at a variety of their sponsored events. Survey responses were collected between March 26, 2005 and March 20, 2006. The survey was open to all nurses. EWG scientists compiled all completed responses from 1,552 nurses from 50 states who reported detailed information on their job and exposure history, health history, and the health of their 2,498 children.
The survey examined exposures to 11 chemicals, chemical groups, or hazardous agents: the high level disinfecting and sterilizing chemicals glutaraldehyde and ethylene oxide; medications, including antiretroviral and chemotherapeutic agents; hazards deriving from medical devices, such as mercury and ionizing radiation; anesthetic gases; natural rubber latex; hand and skin disinfection products; and housekeeping chemicals.
EWG scientists conducted standard statistical analyses of the data, assessing the incidence of health effects known or suspected to be associated with each category of exposure by comparing rates of these effects from among nurses reporting high exposures (frequent and of long duration) against nurses with lower reported exposures. Analysis revealed a striking concordance between survey findings and the health risks expected from a review of the open scientific literature with respect to the exposures assessed. Remarkably, for almost none of these hazardous substances are mandatory safety standards in place to protect nurses — any exposure, no matter how high, is legal.
Nurses face daily, chronic exposures to complex mixtures of chemicals and hazardous agents
The exposure assessment reveals that nearly all nurses face long-term exposures to diverse mixtures of chemicals and other hazardous agents, many of which are never tested for safety. Exposures to hazards are widespread, and typically occur in combination over many years:
- 32 percent of nurses report frequent exposure (at least twice weekly) to combinations of at least five chemicals and other hazardous agents for ten years or more.
- 52 percent of nurses report regular (at least once weekly) exposure to combinations of at least six chemicals and other hazardous agents for five years or more.
All but eight of the 1,552 nurses surveyed report exposures during their nursing careers to one or more of 11 hazardous chemicals, agents, or products included in the survey, and 10 nurses were exposed to combinations of at least 15 chemicals or agents at least twice a week for at least 10 years. Many nurses indicate long spans of their careers in which they were exposed to combinations of chemicals and agents that raise concerns, including the one of every 15 nurses surveyed who report exposures to combinations of sterilizing agents, waste anesthetic gases, and radiation at least weekly for at least five years.
These diverse exposures should come as no surprise to anyone in the health care community, or to anyone who has been a patient at a hospital or clinic for any length of time. What is surprising, though, is the lack of mandatory protections in place for nurses. Instead, health care workers must rely on their employers to implement voluntary controls, and to choose safer products, even when more hazardous alternatives may be less expensive or more commonly used.
Untested, low-dose mixtures of chemicals and hazardous agents. In this survey nurses report frequent, long-term exposures to compounds and agents for which exposures are typically legal at any level. Anesthetic gases leak from complex anesthesia machines and from a patient's exhaled breath into operating and recovery rooms where adequate ventilation is not mandatory (NIOSH 1994). Disinfecting and sterilizing agents, linked to allergies and cancer, volatilize and aerosolize into hospital air when equipment is disinfected with these chemicals (EPA 2002 & 2006a, Van Miller et al. 2002, NTP 2004, HCWH 2006). Housekeeping chemicals can build up on surfaces and in the air each time cleaning or disinfecting occurs, and may lead to asthma, allergies, and other, more serious health problems (GS 2004, HCWH 2004 & 2006).
Residues of hazardous medications cover chairs, tables, and counter tops throughout the hospital as a result of nurses administering these therapeutic agents in poorly ventilated areas (Minoia et al. 1998, Connor et al. 1999, Pethran et al. 2003). Latex gloves spur severe, debilitating allergies including anaphylaxis in some nurses (NIOSH 1997). Mercury-containing equipment breaks, spreading mercury vapors through the air of a room where a nurse works and breathes (OSHA 2006). When a nurse cleans or moisturizes a patient's skin or hair with personal care products, the products used contain ingredients that may be hazardous and that are never required to be tested for safety (EWG 2005), and when a nurse disinfects skin and hands to protect against the spread of infectious disease, she or he is exposed to additional chemicals that are also largely without safety limits (EWG 2005).
It is not surprising to find that most nurses feel unprotected at their workplace. In this survey, 46 percent of nurses report feeling that the administrations at their health care facilities are not doing enough to protect them from hazardous exposures, and 37 percent do not think that occupational health is taken seriously at their place of employment. Without safety standards, hospitals should at a minimum educate nurses to protect themselves, but only 38 percent of nurses report that chemical hazards like those mentioned in this survey were part of the occupational health education programs offered at their workplaces.
Nearly one in 10 nursing jobs in the U.S. currently stands open (AACN 2007). Projections show that this gap is expected to grow, as the 40 percent of nurses currently over age 50 begin to retire (ANA 2006); enrollment at nursing schools has not kept pace with this increased retirement rate (AACN 2007). As this country struggles to fill job vacancies and to plan for worse nursing shortages to come, government officials and health care administrators also expect nurses to work increasing numbers of hours, to care for more patients, and to do this in an environment that can be polluted with chemicals and other hazardous agents that have no safety standards and that pose long-term health risks.
To sustain the quality of health care in the U.S., and to encourage new, talented people to enter the nursing field, nurses need mandatory protections that provide them with a healthy and safe environment where they can focus on caring for others, knowing that their own health, and that of their children, will not be at risk in the process.
Recommendations
The government, individual health care facilities, nurses, and patients alike must take action to protect nurses from excess exposures to hazardous substances:
- The government should conduct a long-term, national survey of nurses' health and exposures to chemicals and other hazards, and use this data to regularly assess health risks nurses face from occupational exposures, and to inform efforts to improve safety standards. Those responsible for existing, broad studies of nurses' health should begin to collect data on occupational exposures to chemicals and other hazards. In 2001, the Centers for Disease Control and Prevention announced plans to implement a National Exposures at Work Survey within the health care industry. This survey, which would be repeated every ten years, would provide much needed data on nurses' exposures to hospital hazards, a first step towards identifying those hazards most in need of new or updated safety standards. After extensive preparation, including two pilot studies, funding for the survey has finally been secured. To protect nurses everywhere, we ask that further governmental approval of the study be expedited, so that it can be conducted as soon as possible.
- The government should establish mandatory limits for nurses' exposures to hazardous drugs, chemicals, and agents in the workplace, and should mandate that hospitals phase out the use of hazardous materials, like mercury and latex gloves, that new technologies can render obsolete.
- Health care facilities should act now to replace hazardous materials and to provide engineering controls nurses need to reduce exposures. Hospitals should phase out mercury-containing equipment, replace or control hazardous sterilizing agents, construct ventilation systems to clear waste gases from the air, and phase out latex gloves. They should monitor the air, surfaces, and even nurses' bodies for chemicals. They should educate nurses on the hazards and safe use of chemicals and other hazardous agents. And they should not wait for these actions to be mandatory.
- Nurses should work within their own facilities to catalyze these changes and reduce their own exposures.
- Patients should begin to ask their health care providers about programs in place designed to reduce a hospital or other health care facility's use of hazardous materials. Any such programs will protect not only nurses, but also patients, who can be exposed to the same chemicals that nurses contact day after day.
Nurses are exposed not only to chemicals used in the workplace, but also to trace contaminants in food, air, water and ingredients in consumer products. Studies of ordinary people indicate that typical Americans are contaminated with low levels of a range of man-made chemicals (e.g. EWG 2003). For almost none of these chemicals is the manufacturer required to conduct even the most basic of safety studies. Nurses' total body burden of chemicals, and ultimately the health risks these exposures impart, stem from these complex mixtures of largely untested, low doses of industrial and occupational chemicals.
Nurses' exposures demonstrate that dramatic improvements will require measures that go beyond those that would protect nurses from hospital exposures. Far-reaching reform is needed to overhaul an outdated system of public health protections, laid out in the 1976 Toxic Substances Control Act, that allows broad exposures to chemical mixtures, beginning even before the moment of birth, with largely unknown consequences to human health. This Act is the only major public health and environmental statute that has never been updated (GAO 1994 & 2005). Its reform should be a priority for anyone devoted to protecting public health.
Table 1. Study details - Nurses with high exposures report elevated rates of cancer and birth defects among their children |
||||
| Increased incidence in children of nurses with high exposure during pregnancy (versus low or no exposure) | High exposure during pregnancy: Nurses' children with the listed health problem (values in parentheses are scaled to per 1,000 children) | Low exposure during pregnancy: Nurses' children with the listed health problem (values in parentheses are scaled to per 1,000 children) | Selected supporting studies | |
|---|---|---|---|---|
| Cancer among nurses' children | ||||
| Radiation | 36% | 5 of 466 (11 of 1,000) | 16 of 2,023 (8 of 1,000) | Studies from several countries indicate that past radiographic examinations of the abdomens of pregnant women produced an increased risk of development of childhood cancer of about 40 percent (Doll and Wakeford, 1997). Nurses' risk of having children stricken with cancer from occupational radiation exposures in utero has never been studied. |
| Birth defects (all types) among nurses' children | ||||
| Medications, all types | 74% | 63 of 751 (84 of 1,000) | 84 of 1,738 (48 of 1,000) | A study of nurses in Finland revealed rates of birth defects 4.7 times higher for those handling chemotherapeutic agents, based on eight cases (Hemminki et al. 1985). |
| Antineoplastic drugs | 67% | 29 of 319 (91 of 1,000) | 118 of 2,170 (54 of 1,000) | |
| HIV (antiretroviral) drugs | 82% | 29 of 296 (98 of 1,000) | 118 of 2,193 (54 of 1,000) | |
| Housekeeping chemicals | 97% | 63 of 687 (92 of 1,000) | 84 of 1,802 (47 of 1,000) | |
| Musculoskeletal defects among nurses' children | ||||
| Glutaraldehyde | 639% | 6 of 206 (29 of 1,000) | 9 of 2,283 (4 of 1,000) | Animal studies indicate glutaraldehyde and ethylene oxide exposures in utero may cause birth defects of the musculoskeletal system (Marks et al. 1980, NTP 1987, Rutledge and Generoso 1989). Studies of this effect among children of nurses exposed to disinfecting and sterilizing agents are needed. |
| Ethylene oxide | 639% | 6 of 206 (29 of 1,000) | 9 of 2,283 (4 of 1,000) | |
| Anesthetic gases | 824% | 8 of 274 (29 of 1,000) | 7 of 2,215 (3 of 1,000) | Animal studies indicate exposures to anesthetic gases in utero may cause birth defects of the musculoskeletal system (Fujinaga et al. 1991). More studies of the health of children of nurses and other health workers exposed to anesthetizing agents are needed. |
|
Notes: "High exposure" refers to reported exposure frequency of at least once weekly during pregnancy. "Low or no exposure" refers to all other, lower reported exposure frequencies. |
||||
Table 2. Study details - Nurses with high exposures report elevated rates of cancer, asthma, and miscarriage |
||||
| Increased incidence in nurses with high exposure (versus low or no exposure) | High exposure: Number of nurses with the listed health problem (values in parentheses are scaled to per 1,000 nurses) | Low exposure: Number of nurses reporting the listed health problem (values in parentheses are scaled to per 1,000 nurses) | Selected supporting studies | |
|---|---|---|---|---|
| Cancer | ||||
| Medications, all types |
14% | 103 of 777 (133 of 1,000) | 90 of 775 (116 of 1,000) | Many pharmaceuticals, notably antineoplastic drugs used to treat cancer, can themselves cause cancer. The International Agency for Research on Cancer has classified 36 antineoplastic drugs as known, probable, or possible human carcinogens (Connor et al. 2006). The few available studies of nurses have found elevated rates of leukemia and chromosome damage associated with exposures to antineoplastic drugs (Martin 2005). |
| Antineoplastic drugs | 42% | 27 of 159 (170 of 1,000) | 166 of 1,393 (119 of 1,000) | |
| Breast Cancer | ||||
| Radiation | 22% | 10 of 264 (38 of 1,000) | 40 of 1,288 (31 of 1,000) | Three studies of a nationwide cohort of over 140,000 radiological technologists indicate elevated risk of breast cancer in women (Doody et al. 1998, Mohan et al. 2003, Sigurdson et al. 2003). Nurses' risk of breast cancer from radiation exposures has never been studied. |
| Asthma | ||||
| Glutaraldehyde | 46% | 38 of 304 (125 of 1,000) | 107 of 1,248 (86 of 1,000) | In a study of health care workers with work-related asthma in four states, nine percent reported that glutaraldehyde triggered asthma symptoms (Pechter et al. 2005). Respiratory therapists using glutaraldehyde were three times more likely to report asthma as those who did not (Dimich-Ward et al. 2004). 3,650 health care workers surveyed in Texas, including 941 nurses, were 2.22 times more likely to develop asthma if they sterilized instruments in the workplace (Delclos et al. 2006). |
| Ethylene oxide | 45% | 14 of 110 (127 of 1,000) | 127 of 1,442 (88 of 1,000) | |
| Housekeeping chemicals | 47% | 70 of 623 (112 of 1,000) | 71 of 929 (76 of 1,000) | In a study of health care workers with work-related asthma in four states, 24 percent reported that cleaning products triggered asthma symptoms (Pechter et al. 2005). 3,650 health care workers surveyed in Texas, including 941 nurses, were twice as likely to develop asthma if they performed general cleaning tasks as part of their jobs (Delclos et al. 2006). |
| Latex | 39% | 85 of 783 (109 of 1,000) | 60 of 769 (78 of 1,000) | Natural rubber latex is a widely recognized asthmagen. A survey of 3,650 health care workers in Texas, including 941 nurses, revealed that the likelihood that these workers developed asthma during their careers was 2.17 times greater if they used powdered latex gloves during years 1992 to 2000 (Delclos et al. 2006). |
| Miscarriage | ||||
| Ethylene oxide | 24% | 33 of 110 (300 of 1,000) | 350 of 1,442 (243 of 1,000) | Nurses performing sterilizing procedures during pregnancy were three times more likely to experience miscarriage than other nurses, according to a study of Finnish hospital staff. Increased miscarriage was linked specifically with exposure to ethylene oxide, as opposed to other sterilizing agents (Hemminki et al. 1992). |
| Medications, all types | 19% | 208 of 777 (268 of 1,000) | 175 of 775 (226 of 1,000) | Studies of health care workers from three different countries revealed rates of miscarriage 1.5 to 2.3 times higher for those who handled antineoplastic medications while pregnant, as compared to those who did not (Selevan et al. 1985, Stücker et al. 1990, Valanis et al. 1999). |
| Antineoplastic drugs | 14% | 44 of 159 (277 of 1,000) | 339 of 1,393 (243 of 1,000) | |
|
Notes: "High exposure" refers to reported exposure frequency of at least once a week for at least 10 years. "Low or no exposure" refers to all other, lower reported exposure frequencies. |
||||
Nurses' Exposure
Nurses' Workplace Exposures
Environmental Working Group, Health Care Without Harm, the American Nurses Association, and the Environmental Health and Education Center of the University of Maryland's School of Nursing conducted a survey on hazardous exposures and the health of nurses nationwide. 1,552 nurses responding to the survey reported exposures to numerous chemicals and other hazards found in hospitals. Exposures to hazards were widespread, and typically occurred in combination over many years:
(*Exposure was considered frequent if it occurred at least 2-3 times per week, and regular if it occurred at least once per week. In this study, "high" exposure is classified as exposure at least once per week for at least ten years.)
- 32 percent of nurses reported frequent* exposure to combinations of at least five chemicals and other hazardous agents for ten years or more.
- Half of nurses reported regular* exposure to combinations of at least six chemicals and other hazardous agents for five years or more.
The cumulative health risks to nurses from their long-term exposures to complex mixtures of chemicals and other hazardous agents have never been studied. Many investigations, however, show that chemicals in combination can be more toxic than would be predicted based on studies of the chemicals singly. For example, a government study of the HIV drug AZT, in combination with another medication commonly prescribed to patients with AIDS, found a far greater than expected level of blood damage when the two were given to mice simultaneously (NIEHS 1998).
The unexpected and unexplained synergistic effect produced by this combination of drug therapies suggests that nurses too may experience health effects difficult to predict based on studies of each chemical exposure individually. This survey did not take into consideration the impact of mixed or combined chemical exposures, a serious issue because most nurses are exposed to multiple chemicals in the workplace at the same time. There is a critical need for research evaluating the combined impact of chemicals on the human body, analogous to studies of the potential health impacts of combinations of pharmaceutical agents in patients.
When speaking on indoor air pollutants like those commonly found in hospitals, an EPA official noted that some people are more susceptible than others to what can be very low levels of exposure: "...mainstream medical opinion today would tell you there's no evidence that such low concentrations would cause adverse reactions in people. However, I think a moment's consideration will tell you that people differ in their response to environmental stimuli by many orders of magnitude. And some people are going to react at extremely low concentrations" (Tomlinson and Wallace 1995).
This survey examined 11 specific hazardous exposure categories. These included the high level disinfecting and sterilizing chemicals glutaraldehyde and ethylene oxide; medications, including antiretroviral and chemotherapeutic agents; hazards deriving from medical devices, such as mercury and ionizing radiation; anesthetic gases; natural rubber latex; hand and skin disinfection products; and housekeeping chemicals. Exposure frequencies reported by nurses who completed this survey are shown in Table 1.
Nurses' Exposures
Table 1: Nurses are exposed to numerous occupational hazards, often lasting a decade or more, and sometimes while pregnant
Summary of nurses' exposures reported in this survey. All percentages are reported relative to the entire surveyed nurse population.
| Hazardous Exposure | Any On-the-Job Exposure | Regular Exposure for at least Ten Years | Any Exposure While Pregnant |
|---|---|---|---|
| Anesthetic gases | 36% | 11% | 12% |
| Antiretroviral medications | 47% | 11% | 13% |
| Chemotherapeutic agents | 41% | 10% | 13% |
| Ethylene oxide | 29% | 7% | 9% |
| Glutaraldehyde | 52% | 20% | 16% |
| Hand and skin disinfection | 96% | 53% | 30% |
| Housekeeping chemicals | 92% | 40% | 29% |
| Ionizing radiation | 53% | 17% | 19% |
| Latex | 94% | 50% | 30% |
| Medications | 95% | 50% | 31% |
| Mercury-containing devices | 77% | 36% | 27% |
It is not surprising that over 90 percent of nurses report workplace exposure to the four most commonplace health care hazards: hand and skin disinfection products, medications, housekeeping chemicals, and latex.
Perhaps more surprisingly, one in five nurses responding to this survey reported regular exposure to glutaraldehyde for at least ten years. Glutaraldehyde is an allergen (Takigawa and Endo 2006), an irritant (Takigawa and Endo 2006), and a suspected asthmagen (Delclos et al. 2006, HCWH 2006), a chemical that can cause those exposed to develop asthma. Animal studies link glutaraldehyde exposure to a number of other health effects, ranging from anemia (Bandman et al. 1994) to leukemia (Van Miller et al. 2002).
One in five nurses reported exposure to ionizing radiation while pregnant. Studies of childhood cancer indicate increases in cancer development in children exposed to low levels of ionizing radiation in utero (Cox et al. 1995, Doll and Wakeford 1997). The National Academy of Sciences Board on Radiation Effects Research (BRER), an authority on the risks associated with occupational exposures to ionizing radiation, considers no exposure to be too low to produce potential health effects (Prasad et al. 2004, BRER 2006).
Examples like these highlight the high frequency and lengthy duration of exposures of many nurses to numerous hospital hazards. Forty-six percent of nurses responding to the survey felt that the administrations at their health care facilities were not doing enough to protect nurses from hazardous exposures. Only 38 percent of nurses reported that chemical hazards like those mentioned in this survey were part of the occupational health programs offered at their workplaces. Armed with the information provided on this site, nurses can advocate for change to reduce their exposure to toxins in their places of work, improving their health and the health of their patients. Of the 11 exposure categories included in this survey, three are highlighted below.
Hazardous medications. Studies that measure residues of medications in nurses' urine indicate widespread exposures to fugitive particles and vapors, even among nurses who don't prepare and administer drugs (NIOSH 2004). Wipe samples from 14 studies show ubiquitous contamination of work surfaces with drug residues, including floors, counter tops, storage areas, and even tables and chairs in patient waiting areas (NIOSH 2004). Nurses are exposed when they touch these surfaces. In addition, they are exposed directly when they breathe vapors and particles as they prepare drugs, expel air from syringes, sort capsules, handle drug containers, or even when they clean a patient's body fluids.
One nurse in this study, who completed an optional survey section tracking potential exposures over a single shift, reported that among all her other types of exposures she also prepared and delivered 19 separate medications, some for multiple patients, that included capsules, intravenous medications, patch medications, gels, liquids, and aerosols.
Although the National Institute for Occupational Safety and Health (NIOSH) acknowledges that "it is known that exposures to even very small concentrations of certain drugs may be hazardous for workers who handle them or work near them," the government has yet to set enforceable limits for nurses' exposures to drugs for any but a few of the nearly 5,700 drugs approved by the FDA (NIOSH 2004); does not mandate that hazardous drugs be prepared in controlled, carefully ventilated environments; and has issued only a guidance document in lieu of standards that would protect nurses from exposures to the hazardous drugs their jobs routinely require them to handle (NIOSH 2004).
Latex. In the decade following Centers for Disease Control and Prevention's (CDC) 1987 recommendation for universal precautions for health care workers to protect against the spread of AIDS, the use of latex gloves in the U.S. soared from a rate of two billion to nine billion pairs each year (Tillotson 1997). Though still the industry standard for gloves, latex is now known to be a potent allergen. NIOSH estimates that 8 to 12 percent of all health care workers have become allergic to latex (NIOSH 1997), with reactions ranging from skin irritation to asthma and anaphylactic shock. Nurses with an allergy to latex have trouble avoiding exposure: Latex is used not only in gloves, but also in catheters, blood pressure cuffs, anesthesia equipment, and even balloons, pencil erasers, and lingerie elastic.
OSHA now mandates that facilities provide alternatives to latex for workers who develop allergies (29 CFR 1910.1030(d)(3)(iii)), but does not require replacement of latex products to prevent allergies in the first place. OSHA continues to allow the use of powdered latex gloves, even though the latex protein allergens bind to the powder, significantly increasing allergy risks for nurses who inhale powder that becomes airborne when gloves are removed (NIOSH 1997). Work in health care facilities can become impossible for nurses who develop severe allergies from latex.
NIOSH recognizes the potential severity of latex reactions, noting that "in some instances, sensitized employees have experienced reactions so severe that they impeded the worker's ability to continue working in their current job" (NIOSH 1997). A review in the journal Nursing gives a more direct assessment: "More than a minor annoyance, a severe latex allergy could end your career" (Lenehan 2002). Latex allergy is a preventable disease that is completely avoidable, but still prevalent among nurses because of the resistance of the government and health care facilities to require the use of widely-available latex alternatives.
Mercury. Although mercury is a widely-recognized, potent neurotoxin, hospitals and other health care facilities across the country continue to use mercury-containing equipment like thermometers and sphygmomanometers. The government continues to allow these uses even though cost-effective alternatives are widely available. When mercury devices break, the mercury vaporizes. Nurses can inhale these vapors, allowing efficient absorption of mercury through the lungs to the bloodstream and then to the brain. Although this survey did not collect data on nurses' exposures to broken mercury instruments, it did gather information on how often and over how many years of their career they used mercury-containing devices. Analysis revealed that more than one-third of all nurses used mercury devices routinely (at least once weekly) for ten years or more.
A typical large hospital might have over one hundred pounds of mercury on-site, contained within hundreds of devices throughout the facility, unless it has taken specific steps to replace mercury-containing equipment (HERC 2004). A large hospital in Los Angeles documented about 18 mercury spills each year, and estimated cleanup costs as $10,000 per year in labor alone (EPA 2002). The cost of replacing mercury-containing devices is modest in comparison. No federal regulations mandate mercury phase-outs in hospitals. Instead, OSHA has set an enforceable exposure limit for nurses that is five times the level known to lead to neurological symptoms after several years of occupational exposure.
Are Nurses Protected?
Occupational Safety and Health Regulations and Nurses' Health
Employing over 12 million people, health care is the second-fastest-growing sector of the U.S. economy (NIOSH 2006). Hospitals and other health care facilities provide jobs for 1.6 million workers at 21,000 work sites (OSHA 2006). Yet while caring for the health of their communities, every health care worker may be exposed to numerous occupational hazards every day. Unfortunately, many of the regulations aimed at protecting these workers are obsolete, and enforcement of existing requirements is inadequate.
Table 1: Few regulations limit nurses' exposures to hazards in the workplace
| Chemical or hazardous agent and key health concerns | Mandatory limits for nurses' exposures? | Does the gov't product approval consider nurses' exposures and safety? |
|---|---|---|
| Anesthetic gases (miscarriage, birth defects) | No | No |
| Antiretroviral medications (unknown health effects) | No | No |
| Chemotherapeutic agents (birth defects, cancer) | Only for platinum- and arsenic-based drugs; rarely monitored or enforced | No |
| Ethylene oxide (miscarriage, cancer) | Yes (OSHA Permissible Exposure Limit) | No |
| Glutaraldehyde (skin and eye problems) | No | No |
| Hand and skin disinfection (skin allergies, asthma) | Only for isopropyl alcohol (OSHA Permissible Exposure Limit) | No |
| Housekeeping chemicals (asthma, allergies) | No | No (no approval process for most products) |
| Ionizing radiation (cancer) | Yes (maximum exposure limit) | No |
| Latex (asthma, allergies, anaphylaxis) | No | No |
| Mercury-containing devices (neurological effects) | Yes (OSHA Permissible Exposure Limit) | No |
| Medications (birth defects, miscarriage) | No | No |
| Personal care products (dermatitis, cancer) | No | No (no approval process) |
The U.S. Department of Labor's Occupational Safety and Health Administration (OSHA) is charged with developing and enforcing regulations designed to protect workers. Though OSHA has devoted rigorous attention to regulations concerning bloodborne pathogens, many hazards commonly found in health care settings have received far less scrutiny. In fact, of 12 key hazardous exposures examined, OSHA has set health-based exposure limits for just three (ethylene oxide, ionizing radiation, and mercury), and has set limits that cover just a small fraction of chemicals in two other exposure categories (cancer drugs and skin disinfectants). None of these limits have been updated within the last two decades.
Government enforcement of existing occupational safety and health regulations within health care settings is disturbingly inadequate. Over one full year, from October 2000 to September 2001, OSHA performed just 103 hospital inspections while overseeing more than 5,800 hospitals nationwide (NCHS 2005, OSHA 2006). By inspecting a tiny fraction of health care facilities for violations of regulations designed to protect nurses and other health care workers, OSHA is failing to protect millions of Americans from occupational hazards.
Federal regulations and guidelines
OSHA has established exposure limits (Permissible Exposure Limits, or PELs) for a few specific exposures relevant to the hospital environment, including ionizing radiation (29 CFR 1910.1096), used for diagnostic imaging, radiotherapy, or produced by radioactive medicines; ethylene oxide (29 CFR 1910.1047), a powerful cold sterilant; mercury (29 CFR 1910.1000), a component in a variety of medical devices; isopropyl alcohol, (29 CFR 1910.1000) an important disinfectant; and a few other chemicals. These exposure limits, however, were set over 20 years ago, and have not been tightened despite recent scientific evidence that has led to increasing concern regarding the potential health effects of chronic, low-dose occupational exposures to these hazards.
Further regulations relevant to health care settings include those regarding hazard communication, involving the labeling of hazardous chemicals, training of employees on proper use of chemicals, and maintaining available chemical safety and health information in the form of a collection of material safety data sheets (MSDS) (29 CFR 1910.1200). Health care facilities are obligated to provide appropriate personal protective equipment to their staff (29 CFR 1910 Subpart I), and to provide alternatives to latex for staff with latex allergy (29 CFR 1910.1030(d)(3)(iii)). Facilities employing mercury-containing devices must also provide spill kits for the safe cleanup of mercury spills (29 CFR 1910.132 and 1910.134). Staff exposure to ionizing radiation must be monitored and recorded (29 CFR 1910.1096). In addition, EPA evaluation and registration of pesticides, especially antimicrobial disinfectants used in health care settings, prevents some harmful chemicals from being used in hospitals.
There are many chemicals in common use in health care settings, however, that are not regulated by OSHA or EPA standards. For these chemical hazards, any exposure is legal, and the burden falls on individual health care facilities to establish safe workplace practices for employees. For example, while OSHA has announced plans for over ten years to develop exposure limits for glutaraldehyde (SH 2006), a high level disinfecting agent known to trigger asthma and contact dermatitis, no deadline has been set. As well, established concerns regarding cancer and reproductive problems linked to the exposure of health care workers to trace amounts of multiple, powerful hazardous medications have resulted in no new regulatory efforts by OSHA (NIOSH 2004).
The National Institute of Occupational Safety and Health (NIOSH), an agency within the Centers for Disease Control and Prevention (CDC), studies a variety of occupational issues relevant to health care, and formulates guidelines concerning handling of hospital hazards. These guidelines, however, are not enforceable, and studies indicate adherence to them within medical centers is often sporadic. For example, concentrations of the anesthetic gas nitrous oxide in dental operatories often exceed the limits recommended by NIOSH, even when appropriate scavenging equipment is in use (NIOSH 1994). Many nurses and other health care workers who prepare and administer hazardous medications, or care for patients treated with these medications, do not use the recommended personal protective equipment outlined by NIOSH (Valanis et al. 1991 & 1992, Mahon et al. 1994, Nieweg et al. 1994, Martin and Larson 2003).
At this time, primary responsibility for many aspects of health care worker health and safety lies with the administration of individual hospitals and other health care facilities. Caring, motivated staff can use resources from NIOSH, as well as nongovernmental organizations such as Health Care Without Harm, Hospitals for a Healthy Environment (H2E) and ANA's Center for Occupational and Environmental Health, to create programs that reduce employee exposures to hazards above and beyond OSHA requirements. These programs may facilitate use of less hazardous substitute chemicals, encourage more efficient use of hazardous chemicals, implement engineering solutions that reduce or prevent exposures to health care workers, or improve training, documentation, and investigation of exposure incidents.
OSHA has implemented a Voluntary Protection Program that encourages medical centers to establish their own internal regulations regarding hazardous exposures and other occupational health and safety concerns (OSHA 2000). The Administration has concluded that effectively managing safety and health protection programs improves employee morale and productivity, and significantly reduces workers' compensation costs and other less obvious costs of work-related injuries and illnesses (OSHA 2006). Despite the clear benefits of these measures to health care personnel and hospital efficiency, there has been no effort to require such plans for all health care facilities.
Perhaps the best drivers of efforts to improve the safety and health of occupational environments are careful epidemiological studies of worker health and exposures to a variety of hazards. Unfortunately, in recent years neither OSHA nor any other U.S. agency has performed an epidemiological study of nurses and other health care workers with respect to exposures to hazardous chemicals. In 2001, the Centers for Disease Control and Prevention announced plans to implement a National Exposures at Work Survey within the health care industry. This survey would provide much needed data on nurses' exposures to hospital hazards, a first step towards identifying those hazards most in need of new or updated safety standards. After extensive preparation, funding for the survey has finally been secured. We ask that further governmental approval of the study be expedited, so that it can be conducted as soon as possible.
Lacking this data, it is difficult to prioritize health-based improvements to existing hazardous exposure limits, or identify new concerns regarding any of the broad range of exposures present in the hospital setting. Thus, well-designed studies that probe the effects of hazards on the health of health care personnel would generate information that could guide future efforts to ensure the occupational safety and health of this vital segment of the population.
Health care workers spend their lives healing the ill and the injured. They deserve to work in an environment that is safe and healthy. To foster an environment free of hazards, OSHA must:
- update existing regulations concerning well-established hazardous exposures;
- mandate development and implementation of hospital and health care worker protection plans that include many of the guidelines and best practices outlined by NIOSH;
- increase enforcement efforts;
- conduct epidemiological research on the effects of hazardous exposures on health care workers' health.
The System is Broken
The safety of chemical mixtures, including the unique mixtures to which nurses are exposed, is unknown — no safety testing is required.
Environmental Working Group studies have documented the presence of 469 chemicals in the blood, urine, and breast milk of 94 people tested, with diverse mixtures of up to hundreds of industrial chemicals, pesticides, and other pollutants in each person (e.g. EWG 2005). These exposures, called the "body burden" of chemicals, stem from contaminants in food, air, tap water, and even house dust, and also from ingredients in consumer products. People inhale these chemicals, ingest them, or absorb them through the skin.
Nurses are exposed not only to the range of chemicals found in these studies, but also to the many chemicals used in hospitals and other health care facilities. And while some health care chemicals (like drugs) have been tested for safety, the same is not true for industrial chemicals used in consumer products and found in people everywhere:
- The complex mixtures of chemicals in the human body have never been tested for safety.
- Even singly, chemicals are rarely tested — what's done is voluntary.
- For chemicals invented 50 years ago or last month, the story is the same: No required testing.
Most people assume chemicals in consumer products are thoroughly tested before they are sold. But for nearly all chemicals, there is no requirement that manufacturers test their products for health effects at any stage of production, marketing, and use (Wilburn 2005). Under the Toxic Substances Control Act, the law that regulates industrial chemicals in the United States, chemical companies can put new compounds on the market with no studies of their effects on people or the environment (GAO 1994 & 2005).
When the Toxic Substances Control Act was passed in 1976, EPA grandfathered in 63,000 chemicals presumed safe or slated for review. Since then, EPA has reviewed the safety of only a small fraction:
- EPA has not reviewed or even begun gathering safety data for more than 80 percent of the 15,000 chemicals produced or imported in annual quantities exceeding 10,000 pounds.
- Through a voluntary program, chemical manufacturers submit screening studies on nearly 3,000 chemicals people are most likely to be exposed to. EPA, however, has no plan on how to use this data to assess public health risks.
Under current law, companies debut new consumer product chemicals in a 90-day "Premanufacturing Notification" process (EPA 1997). EPA approves the vast majority of submissions with no restrictions, and in more than half of all cases, in the complete absence of toxicity data.
- Fewer than half of all applications to the EPA for new chemicals include any toxicity data.
- The government approves 80 percent with no restrictions, usually in less than three weeks.
- Any data provided are cursory, because the government lacks authority to request more.
- If there are no data, the government uses chemical models — widely acknowledged to be inaccurate — that estimate harm to human health or the environment.
In addition to their everyday exposures to consumer product chemicals that haven't been tested for safety, nurses are also exposed to an array of unregulated hazards found in hospitals. Thus, nurses experience unique exposures that raise serious questions about potential health impacts. These exposures also argue for broad changes that would address not only nurses' exposures in hospitals, but the full scope of their exposures.
What You Can Do
• 5 Steps You Can Take
• Useful Resources
• Suggested Reading
5 Steps You Can Take
Strategies for Improving Environmental Health in Your Hospital
1. Know your workplace rights.
The Hazard Communication Standard (also known as the Worker Right to Know Law) says employers must:
- Maintain a set of Material Safety Data Sheets (MSDS) for chemical products used in your workplace. Each MSDS must list the names of the chemical ingredients in products, the potential health effects associated with exposure to the chemical, physical hazards like flammability and corrosivity, appropriate protective measures like gloves and eye protection, and emergency information (including the number of someone to call in case of emergency).
- Provide training on the health and safety risks that may be posed by potential hazardous chemical exposures in the workplace to all employees.
- Retrain or supplement training if you're moved to a new area or when new chemicals are introduced.
- Create a written Hazard Communication policy that describes how all the elements of the standard will be satisfied.
2. Share your story
- Tell us about your experience.
- Join or start a committee on health and safety, the environment of care, purchasing and product safety, or environmental concerns.
- Bring up your concerns at staff meetings, unit leader meetings, or departmental meetings.
3. Advocate for chemical safety
- Encourage the adoption of strong and enforceable chemical policy at the federal level.
- Help change practices to reduce exposures in your health care facility by encouraging the development of broad chemical policy.
- Participate in policy changes at the local, state and federal levels to address chemical exposures and environmental health concerns.
- Improve the quality, accuracy and utilization of the Material Safety Data Sheets (MSDS) -- here's how.
4. Create change in your facility
- Work with facility administrators to encourage the adoption of broad chemical policy.
- Wherever possible, use an alternative to the most hazardous chemicals.
- Educate staff before introducing new chemicals.
- Make sure that safety control measures are in place for new and established chemicals.
- Encourage the annual survey of all chemicals used within each unit, ensuring products are labeled appropriately and that the correct MSDS are available.
- Discourage the use of unnecessary fragrances in health care products, which can affect patients, nurses, and other caregivers.
- Request that your health care facility conducts periodic air and wipe sampling of the nurses' and patients' environments to identify potential hazards.
- Encourage your hospital to join Hospitals for a Healthy Environment (H2E), and volunteer to be your hospital's H2E Nurse Liaison.
5. Educate and be educated
- Call Health Care Without Harm, Hospitals for a Healthy Environment, ANA's Center for Occupational and Environmental Health, or University of Maryland Environmental Health Education Center to request a speaker to give a presentation at your health care facility.
- Organize a nursing grand rounds on environmental health issues.
- Work with the nurses in charge of education and professional development at your facility to provide educational programs on environmental health issues.
- Educate patients, family and friends to help spread the word about the impact of the environment on health and well-being and encourage them to take action.
Tips and Useful Resources:
These sites will help you choose safer products for your facility:
- Sustainable Hospitals provides a listing of some of the most hazardous products that are used in health care and a listing of alternatives, when they are known.
- The Risks to Asthma Posed by Indoor Health Care Environments Report from has a good list of alternatives and methods for reducing exposure to chemicals that are either asthmagens or asthma triggers.
- ANA's Center for Occupational and Environmental Health
- Women's Health
- Science
- Environmental Health Initiative [http://www.ehinitiative.org/] of the American Association of Intellectual and Developmental Disabilities
More Useful Resources:
• Agency for Toxic Substances and Disease Registry
www.atsdr.cdc.gov
The mission of the Agency for Toxic Substances and Disease Registry (ATSDR) is to serve the public by using the best science, taking responsive public health actions, and providing trusted health information to prevent harmful exposures and disease related to toxic substances.
• ANA's Center for Occupational and Environmental Health
www.nursingworld.org/MainMenuCategories/OccupationalandEnvironmental.aspx
The Center for Occupational and Environmental Health provides occupational and environmental health expertise on issues related to the nursing professional and health care industry. The mission of the Center is to protect the health and well-being of nurses and their patients and communities through policy advocacy, programs, and training on the prevention and control of occupational and environmental hazards in relation to health care settings.
• ATSDR ToxFAQs
www.atsdr.cdc.gov/toxfaq.html
The ATSDR ToxFAQs is a series of summaries about hazardous substances developed by the ATSDR Division of Toxicology. Information for this series is excerpted from the ATSDR Toxicological Profiles and Public Health Statements. Each fact sheet serves as a quick and easy to understand guide. Answers are provided to the most frequently asked questions (FAQs) about exposure to hazardous substances found around hazardous waste sites and the effects of exposure on human health.
• Beyond Pesticides
www.beyondpesticides.org
Beyond Pesticides (formerly National Coalition Against the Misuse of Pesticides) works with allies in protecting public health and the environment to lead the transition to a world free of toxic pesticides.
• Campaign for Safe Cosmetics
www.safecosmetics.org
The Campaign for Safe Cosmetics is a coalition of public health, educational, religious, labor, women's, environmental and consumer groups. Its goal is to protect the health of consumers and workers by requiring the health and beauty industry to phase out the use of chemicals linked to cancer, birth defects and other health problems, and replace them with safer alternatives. The site provides a list of safer cosmetics.
• Centers for Disease Control National Center for Environmental Health
www.cdc.gov/nceh
The National Center for Environmental Health plans, directs, and coordinates a national program to maintain and improve the health of the American people by promoting a healthy environment and by preventing premature death and avoidable illness and disability caused by non-infectious, non-occupational environmental and related factors.
• Center for Health, Environment, and Justice
www.chej.org
CHEJ's overarching goal has consistently been to prevent harm — particularly among vulnerable populations such as children. If a safer process, material or product exists it should be used. CHEJ believes that everyone, regardless of income, race, religion, or occupation, has a right to live, work, learn, play and pray in a healthy community.
• Childrens' Environmental Health Network
www.cehn.org/cehn/trainingmanual/manual-front.html www.cehn.org/cehn/resourceguide/rghome.html
Links for a training manual and a resource guide on children's environmental health for health professionals in the U.S.
• Children's Health Protection
yosemite.epa.gov/ochp/ochpweb.nsf/content/homepage.htm
This is the Environmental Protection Agency's home page on issues related to the environmental health of children.
• Collaboration for Health and the Environment
www.healthandenvironment.org
CHE is a diverse partnership of individuals and organizations working collectively to advance knowledge and effective action to address growing concerns about the links between human health and environmental factors.
• EnviRN website
www.enviRN.umaryland.edu
EnviRN is dedicated to supporting nursing professionals seeking accurate, timely and credible scientific information on environmental health and nursing. This interactive and dynamic resource seeks to foster the development of a "virtual nursing village" for the sharing of teaching strategies, practice guidance and consensus on future research needs for nursing and environmental health. The ultimate goal is to prevent environmental disease by increasing the numbers of nursing professionals who can recognize environmental etiologies and risk factors of disease, promote health through risk reduction and control strategies and empower individuals, families and communities through partnering, advocacy and education.
• Environmental Health
http://www.nursingworld.org/MainMenuCategories/ANAMarketplace/ANAPeriodicals/OJIN/TableofContents/Volume122007/May31/EnvironmentalHealthImportantChoicesforaGreenerWorld.aspx
EnvironmentalHealthImportantChoicesforaGreenerWorld.aspx
Important Choices for a Greener World by Susan Wilburn. The Online Journal of Issues in Nursing.
• Environmental Health and Toxicology
sis.nlm.nih.gov/enviro/toxtutor.html
A free on-line toxicology tutorial created by the National Library of Medicine.
• Envirotools
www.envirotools.org
This website provides a collection of educational materials on Superfund and Brownfield sites, along with sites cleaned up under state programs. EnviroTools contains presentation visuals, fact sheets, web links, a glossary and an annotated bibliography of other outreach resources, all designed to help cut through the confusion and jargon of site cleanup projects.
• EPA's Envirofacts database
www.epa.gov/enviro
This website is a single point of access to select U.S. EPA environmental data. It provides access to several EPA databases to provide you with information about environmental activities that may affect air, water, and land anywhere in the United States. With Envirofacts, one can learn more about environmental activities in a specific area or generate maps of environmental information.
• EWG's Body Burden Studies
EWG's Human Toxome Site
Provides information on EWG's Human Toxome Project and its various body burden studies of more than 500 chemicals in adults, neonates, children, and mothers and daughters.
• EWG's Food Guide
www.foodnews.org
Learn about the "best and worst" produce and how to buy and eat healthier from EWG's analysis of 40,000 government tests of pesticides in popular fruits and vegetables.
• EWG's National Tap Water Quality Database
EWG's Tap Water Database
EWG has compiled drinking water contamination on over 39,751 water utilities in 42 states through contact with state environmental and health agencies. For the first time ever, you will see how your tap water stacks up against other cities and towns throughout the US.
• EWG's Skin Deep Database on Safe Personal Care Products
Skin Deep
EWG's Skin Deep database, an interactive guide to personal care product safety, pairs ingredients in nearly 25,000 products against 50 definitive toxicity and regulatory databases, making it the largest integrated data resource of its kind. Provides tips on how to shop for less toxic personal care products.
• Food and Drug Administration
www.fda.gov
The FDA is responsible for protecting the public health by assuring the safety, efficacy, and security of human and veterinary drugs, biological products, medical devices, our nation's food supply, cosmetics, and products that emit radiation. The FDA is also responsible for advancing the public health by helping to speed innovations that make medicines and foods more effective, safer, and more affordable; and helping the public get the accurate, science-based information they need to use medicines and foods to improve their health.
• HCWH's The Luminary Project
www.theluminaryproject.org
The Luminary Project: Nurses Lighting the Way to Environmental Health is an effort to capture the illuminating stories of nurses' activities to improve human health by improving the health of the environment. The shining stories and resources on this website come together as a "virtual international community" guiding nurses on how to creatively and strategically address environmental problems and illuminate the way towards safe hospitals, communities with clean air, land and water and children born without toxic chemicals in their bodie
• Health Care Without Harm
www.noharm.org/us
HCWH is an international coalition of over 460 organizations in more than 50 countries, working to transform the health care sector so it is no longer a source of harm to people and the environment.
• Healthy Children Project
www.healthychildrenproject.org/exposures/index.html
The purpose of the Learning Disabilities Association of America's Healthy Children Project is to raise public awareness about potentially harmful toxics and health risks. The project targets women and men of reproductive age (especially those at high-risk), their children, and the health care professionals who serve them to make more informed and safer choices to protect our children and future generations from preventable harm. Take a quiz: www.healthychildrenproject.org/quiz.html
• Healthy Schools
nursingworld.org/mods/archive/mod250/CESAVERS.HTM
Healthy Schools Network, Inc. is a 501 c3 national environmental health organization that does research, information, education, coalition-building, and advocacy to ensure that every child has a healthy learning environment that is clean and in good repair.
• Hospitals for a Healthy Environment (H2E)
www.h2e-online.org
H2E is creating a national movement for environmental sustainability in health care. H2E is based on the vision of a healthy health care system — a system that embraces safer building products, clean air, energy and water efficiency, safe working practices, and a commitment to public health demonstrated through waste volume and toxicity reduction.
• Institute of Medicine Report - Nursing, Health, and the Environment
www.nap.edu/books/030905298X/html/index.html
If environmental health hazards and health effects are to be recognized and dealt with effectively, it is of fundamental importance that all health care providers have a clear understanding of the association between the environment and health. Toward that end, the committee makes a series of recommendations for the integration and enhancement of environmental health in nursing education, practice, and research.
• International Council of Nurses (ICN)
www.icn.ch
ICN is a federation of national nurses' associations (NNAs), representing nurses in more than 128 countries. Founded in 1899, ICN is the world's first and widest reaching international organization for health professionals. Operated by nurses for nurses, ICN works to ensure quality nursing care for all, sound health policies globally, the advancement of nursing knowledge, and the presence worldwide of a respected nursing profession and a competent and satisfied nursing workforce.
• National Institutes of Environmental Health Services
www.niehs.nih.gov
Because environmental exposures contribute substantially to the etiology of many common and complex human diseases, the NIEHS is in a unique position to focus on the interface between environmental exposures, vulnerable populations, human biology and genetics, and the common diseases that limit our longevity.
• Our Stolen Future
www.ourstolenfuture.org
Great information about a new category of toxic chemicals called "endocrine disruptors." Many manmade chemicals fall into this category — chemicals that in some way block, trigger, or change our normal endocrine function.
• Physicians for Social Responsibility (PSR)
psr.org
PSR is a non-profit advocacy organization that is the medical and public health voice for policies to stop nuclear war and proliferation and to slow, stop and reverse global warming and toxic degradation of the environment. (Especially read "In Harm's Way: Toxic Threats to Child Development" available at: psr.igc.org/ihw-download-report.htm)
psr.igc.org/ihw-project.htm
• Resource guide on children's environmental health in U.S.
www.cehn.org/cehn/resourceguide/rghome.html
• Scorecard
www.scorecard.org
This pollution information website provides an in-depth pollution report for one's county, covering air, water, chemicals, and more.
• Sustainable Hospitals
www.sustainablehospitals.org
The Sustainable Hospitals Program is part of The Lowell Center for Sustainable Production. The SHP is located within the University of Massachusetts Lowell, Department of Work Environment. SHP is assisted by faculty, staff, and students of the UMASS Lowell School of Health & Environment and the Massachusetts Toxics Use Reduction Institute (TURI).
• Toxicology Data Network (TOXNET)
toxnet.nlm.nih.gov
The National Library of Medicine's databases for toxic exposures.
• Toxtown US
toxtown.nlm.nih.gov/
An introduction to toxic chemicals and environmental health risks you might encounter in everyday life, in everyday places.
• Union of Concerned Scientists
www.ucsusa.org/
Provides great and provocative reports about a wide variety of environmental issues.
• US Environmental Protection Agency
www.epa.gov
The mission of the Environmental Protection Agency is to protect human health and the environment. Since 1970, EPA has been working for a cleaner, healthier environment for the American people.
Suggested Reading:
A Civil Action by Jonathan Harr
An Inconvenient Truth by Al Gore (2006)
Blue Gold: The Fight to Stop the Corporate Theft of the World's Water by Maude Barlow and Tony Clarke
Chemical Alert: A Community Action Handbook (1993) edited by Marvin S. Legator and Sabrina F. Strawn
Climate Change Begins at Home: Life on the two-way street for global warming By Dave Reay (2005)
Deceit and Denial: The Deadly Politics of Industrial Pollution by Gerald Markowitz and David Rosner
Dying from Dioxin by Lois Marie Gibbs and the Citizens Clearinghouse for Hazardous Waste
Earth in the Balance: Ecology and the Human Spirit by Al Gore
Ecological Medicine: Healing the Earth, Healing Ourselves by Kenny Ausubel, ed.
Environmental Health and Nursing Practice by Barbara Sattler and Jane Lipscomb
Environmental Health: Ecological Perspectives by Kathryn Hilgenkamp
Fast Food Nation by Eric Schlosser
Food Politics: How the Food Industry Influences Nutrition and Health by Marion Nestle
Generations at Risk: Reproductive Health and the Environment by Ted Schettler, M.D., Gina Solomon, M.D., Maria Valenti, and Annette Huddle
Harvest for Hope by Jane Goodall
Having Faith by Sandra Steingraber
Living Downstream: A Scientist's Personal Investigation of Cancer and the Environment by Sandra Steingraber
Not Just a Pretty Face: The Ugly Side of the Beauty Industry by Stacy Malkan (2007)
Nursing, Health, & the Environment: Strengthening the Relationship to improve the Public's Health by the Institute of Medicine, Division of Health Promotion and Disease Prevention, Andrew Macpherson Pope, and Meta A. Snyder
Our Stolen Future: Are We Threatening Our Fertility, Intelligence and Survival? by A Scientific Detective Story Theo Colborn, Dianne Dumanoski, John Peterson Myers
Pediatric Environmental Health (2003) 2nd Ed., American Academy of Pediatrics.
Precautionary Tools for Reshaping Environmental Policy (Urban and Industrial Environments) by Nancy J. Myers (Editor) and Carolyn Raffensperger
Protecting Public Health and the Environment: Implementing The Precautionary Principle by Wes Jackson, Carolyn Raffensperger, and Joel Tickner
Safe Food: Bacteria, Biotechnology, and Bioterrorism by Marion Nestle
Science in the Private Interest: Has the Lure of Profits Corrupted Biomedical Research? by Sheldon Krimsky
Silent Spring by Rachel Carson
The Precautionary Principle in the 20th Century: Late Lessons from Early Warnings
The Ethics of Environmentally Responsible Health Care by Jessica Pierce and Andrew Jameton
The Omnivore's Dilemma: A Natural History of Four Meals by Michael Pollan
The Weather Makers: How Man is changing the Climate and What it Means for life on Earth (2005). By Tim Flannery
Toxic Deception: How the Chemical Industry Manipulates Science, Bends the Law, and Endangers Your Health by Dan Fagin and Marianne Lavelle and the Center for Public Integrity (Corporate Author)
Warnings by David Gee and Timothy O'Riordan
When Smoke Ran Like Water by Devra Davis
About the Survey
Design and Dissemination of the Survey
In collaboration with Health Care Without Harm, the American Nurses Association, and the Environmental Health Education Center of University of Maryland's School of Nursing, Environmental Working Group (EWG) scientists designed an online survey to assess nurses' extent and frequency of exposures to 11 different common health care hazards, as well as the prevalence of a wide variety of health problems among nurses and their children. The survey collected detailed information on job and health history from participating nurses and their children. The survey also collected basic occupational, demographic, and lifestyle data, and probed nurses' attitudes concerning occupational health and their own workplace environments.
The American Nurses Association, Health Care Without Harm, the Environmental Health Education Center of University of Maryland's School of Nursing, and the American Public Health Association's Nurses Section disseminated information about the survey at meetings, conferences, and workshops, and in nursing journals, state nurses associations' newsletters, and specialty nursing organizations' publications. Links to the survey were posted on various nursing websites, including those of the collaborating nursing organizations. Any interested nurse was free to participate in the survey via the website. EWG collected survey responses between March 26, 2005 and March 20, 2006.
Analyzing Survey Data
EWG scientists received complete survey data from 1,552 nurses representing all 50 U.S. states. Eighty percent of respondents were Registered Nurses (RNs); 92 percent were currently working in nursing; and 94 percent were women. The number of years that respondents reported nursing was broadly distributed, with 44 percent of nurses practicing for between 20 and 35 years. Age of respondents was also broadly distributed, with 22 percent reporting an age between 50 and 55 years. Respondents were primarily white/caucasian and non-hispanic (88 percent). Thirty-two percent of respondents had two children, and 42 percent lived in suburban locations. States with a large number of respondents included Florida (80 nurses), Maryland (108 nurses), New York (114 nurses), and Ohio (98 nurses).
EWG scientists analyzed survey responses using basic statistical methods. Researchers assembled information on health effects associated with each hazardous hospital exposure from publicly available government databases, including the Hazardous Substances Data Bank (HSDB) and the Registry of Toxic Effects of Chemical Substances (RTECS), as well as peer-reviewed scientific literature and government publications. Health problems were assessed statistically only if a particular exposure was known or suspected to be its cause. Exposures were examined independently; no attempt was made to assess patterns in exposure to mixed and multiple hazards, although this is an area in need of further research.
EWG researchers assessed health problems among surveyed nurses as a function of exposure duration, comparing nurses reporting exposures at least once a week for at least ten years (high exposure) against all other nurses responding to the survey (low or no exposure). Health problems among the children of surveyed nurses exposed to occupational hazards were assessed as a function of timing of exposure. The prevalence of health effects in the children of nurses exposed at least once per week during pregnancy was compared with the prevalence of health effects in the children of nurses with less frequent or no exposure during pregnancy. This website provides health effects that show an increased prevalence of greater than one percent among highly exposed nurses or their children. In addition, 90 percent confidence intervals were calculated for summary statistics reported in the study summary.
The pool of participants that responded does not necessarily represent a typical cross-section of American nurses, and the survey is subject to recall bias and other common forms of bias. Despite the limitations, the survey does show that many nurses exposed to hazards on the job are experiencing health problems. Remarkably, the government has never conducted a national survey of nurses' health and occupational and environmental workplace hazards, despite the diverse and chronic exposures nurses face. Furthermore, many hospitals have been slow to implement plans to reduce nurses' exposures to hazards. More action and more research are critically needed.
Survey limitations.
Surveys are a well-established epidemiological tool for identifying health risks from occupational exposures to hazards. Several studies of hazardous exposures and the health of health care workers have employed mail-in surveys to collect data (e.g. Hemminki et al. 1982, Valanis et al. 1999, Mohan et al. 2003, Dimich-Ward et al. 2004, Yoshinaga et al. 2005); some also allow for online response to the study questionnaire (e.g. Delclos et al. 2006). Traditional epidemiological surveys are sent to a select group of individuals. Typically, epidemiologists report rates of response to their questionnaires, and often perform statistical adjustments to the data to ensure that it is representative of the entire population of concern.
To reach a broader audience, EWG created an online survey open to anyone interested. While this online format enabled dissemination of the survey to nurses all over the United States, it is not possible to calculate or estimate the response rate. Comparisons to preliminary findings of the National Sample Survey of Registered Nurses (DHHS 2004) suggest that the collection of nurses that chose to respond to the EWG survey may well-represent others in their profession. For example, the average age of nurses in this survey was 47, just as in the national survey; nurses under 40 made up 23.9 percent of the respondents in this survey, while they were 26.6 percent of the national survey. A review of studies on human psychology reveals that internet-based research methods typically produce the same results as traditional methods, providing no evidence for unusual bias among study populations (Gosling et al. 2004).
Some research suggests that those that choose to respond to health surveys like the one presented here may be more likely to have experienced the hazardous exposures and health problems described, or be more aware of the hazardous nature of their work. For example, Axelsson and Rylander (1982) noted that women that were occupationally exposed to anesthetic gas and suffered a miscarriage always responded to a postal survey on the subject, while one-third of women that suffered a miscarriage without being exposed to anesthetic gas did not.
Another issue common to survey-based health data is the accuracy with which respondents report medical information. Nurses are typically better educated about health than the general population, and therefore may provide more accurate information via survey, but this type of "reporting bias" could influence survey findings. Analytical decisions regarding classification of the nurses into high and low exposure categories may also affect survey interpretation. In addition, analyses did not take into consideration confounding factors like exposure to multiple chemicals associated with the same health effect, or other demographic or lifestyle factors that often affect health, such as age, smoking and drinking habits, and day or night shift work; such factors could influence survey results.
While the basic statistical associations reported were not adjusted to account for the potential effects of these types of bias, the associations between hazardous exposures and health outcomes reported demonstrate the need for increased research on nurses' health, and more protective occupational regulations in the health care setting.
About the Survey Partners
Environmental Working Group
Environmental Working Group's research (like Skin Deep and the Shoppers' Guide to Pesticides in Produce) brings to light unsettling facts that you have a right to know. It shames and shakes up polluters and their lobbyists. It rattles politicians and shapes policy. It persuades bureaucracies to rethink science and strengthen regulation. It provides practical information you can use to protect your family and community.
University of Maryland School of Nursing (SON)
The University of Maryland School of Nursing (SON) founded in 1889, is one of the oldest and largest nursing schools, and is ranked seventh nationally. Enrolling more than 1,600 students in its baccalaureate, master's, and doctoral programs, the School develops leaders who shape the profession of nursing and impact the health care environment.
The School of Nursing's Environmental Health Education Center addresses environmental health issues by engaging in education, research, practice, policy and advocacy. The Center's primary focus is on the nursing profession and working collaboratively with community groups, health professionals, advocacy organizations, and government agencies in addressing environmental health challenges.
Health Care Without Harm
Health Care Without Harm is an international coalition of hospitals and health care systems, medical professionals, community groups, health-affected constituencies, labor unions, environmental and environmental health organizations and religious groups.
American Nurses Association
The American Nurses Association is the only full-service professional organization representing the interests of the nation's 2.9 million registered nurses through its 54 constituent member nurses associations. The ANA advances the nursing profession by fostering high standards of nursing practice, promoting the rights of nurses in the workplace, projecting a positive and realistic view of nursing, and by lobbying the Congress and regulatory agencies on health care issues affecting nurses and the public.
